Whether you live in the fast-paced streets of New York City, the tech-driven suburbs of San Francisco, the sprawling urban landscape of Houston, or the ever-busy neighborhoods of Chicago — one thing is increasingly common across every ZIP code in America: people simply can’t sleep. From late-night Netflix binges to early morning commutes, modern American life has been fundamentally redesigned in a way that fights against our natural sleep biology. And the consequences are staggering.
Millions of Americans today deal with the sleeplessness problem on a nightly basis. They toss and turn, stare at the ceiling, check their phones at 2 AM, and still drag themselves out of bed exhausted. This isn’t just occasional restlessness — it’s a growing public health crisis. Insomnia, defined as the persistent difficulty to fall or stay asleep, is now one of the most reported health complaints among adults in the United States.
Eszopiclone 2mg tab is one of the medications that has been commonly used short-term to help treat insomnia in adults who make it hard to fall asleep or stay asleep throughout the night. However, medication is only one part of the picture. Understanding the root causes — how our lifestyles, habits, screen time, and social pressures are rewiring our brains away from healthy sleep — is the first and most important step toward lasting relief.
In this blog, we’ll walk through the real reasons why insomnia is on the rise in America, what Insomnia symptoms to look out for, how modern habits are the primary culprit, and what science-backed strategies can help you reclaim your nights.
The State of Sleep in America Today
According to recent data from the Centers for Disease Control and Prevention (CDC), more than one in three American adults are not getting the recommended seven or more hours of sleep per night. Cities like Los Angeles, Miami, and Atlanta are seeing some of the highest rates of reported sleep disorders in the country. The American Academy of Sleep Medicine has declared insufficient sleep a public health epidemic — and it’s only getting worse.
What makes this particularly alarming is that we’re not just talking about people feeling a little groggy. When you experience disruptions in how you feel or function — when your mood tanks, your focus disappears, your immune system weakens — that’s insomnia making its mark on your daily life. Feeling unrested after sleep, waking up multiple times during the night, and lying awake with racing thoughts are all signs that your body and brain are not getting the recovery they desperately need.
What Exactly Is Insomnia? Understanding the Symptoms
Before we dive into causes, it’s important to clearly understand what insomnia actually looks like. Many people assume insomnia simply means you can’t sleep at all. In reality, it’s much broader than that.
Common Insomnia Symptoms Include:
- Difficulty falling asleep even when you’re exhausted
- Waking up frequently during the night and being unable to go back to sleep
- Waking up way too early in the morning
- Feeling unrested after sleep, even after a full night in bed
- Daytime fatigue, irritability, and difficulty concentrating
- Anxiety about going to bed because you already know you can’t sleep
- Headaches, gastrointestinal problems, and other physical symptoms linked to poor sleep
If any of these sound familiar, you are not alone. Millions of Americans — from busy professionals in Seattle to college students in Boston — silently battle these symptoms every single night. The difference between normal sleep struggles and clinical insomnia is largely about frequency and impact. If your sleeplessness problem is affecting your work, your relationships, or your health consistently, it’s time to take it seriously.
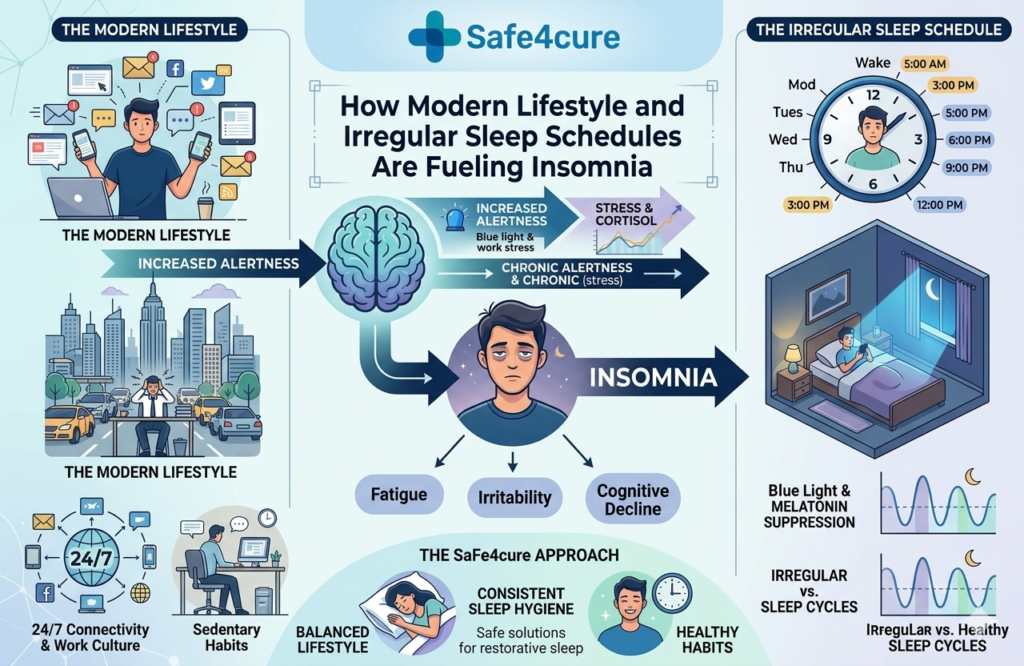
How Modern Lifestyle Is Destroying Our Sleep
1. Screen Time and Blue Light Overexposure
One of the biggest culprits behind America’s insomnia epidemic is the smartphone. The blue light emitted by phones, tablets, laptops, and televisions directly suppresses melatonin — the hormone your body produces to signal that it’s time to sleep. When you’re scrolling through social media or watching YouTube at midnight, your brain literally thinks it’s still daytime. This delays your sleep cycle and can make it hard to fall asleep or stay asleep long after you put the device down.
Research from Harvard Medical School confirms that blue light exposure in the two hours before bedtime significantly delays the natural sleep cycle. In cities like Phoenix or Dallas where nightlife and entertainment culture are deeply embedded in daily routines, people are often exposed to artificial light well past midnight.
2. Irregular Sleep Schedules and Social Jetlag
Modern work culture has completely shattered the consistent sleep routines that humans evolved with over thousands of years. People in Denver might work a 9-to-5 Monday through Friday, then stay up until 3 AM on weekends to socialize — only to crash hard on Sunday and wake up already exhausted on Monday. Scientists call this “social jetlag” and it’s one of the leading causes of chronic insomnia in younger adults.
Your body runs on a biological clock called the circadian rhythm. When you keep shifting your sleep and wake times by several hours across different days, your internal clock gets confused. The result? You can’t sleep when you need to, and you can’t stay awake when you want to.
3. Work-From-Home Culture and Boundary Blurring
Since the pandemic, millions of Americans — particularly in tech hubs like Austin and San Jose — have transitioned to remote work. While this has come with many benefits, it has also completely blurred the boundaries between work time and rest time. People are answering emails at 11 PM, joining early morning calls before the sun rises, and never truly “switching off.” This constant state of mental activation is a recipe for a sleeplessness problem.
4. Chronic Stress, Anxiety, and Hyperarousal
The modern American lifestyle is steeped in stress. Financial pressures, social media comparisons, political anxiety, relationship challenges — all of these activate the body’s stress response system. When cortisol levels stay elevated throughout the day and night, your nervous system remains in a state of hyperarousal. It’s incredibly difficult to drift off to sleep when your brain is wired for fight-or-flight mode.
5. Caffeine, Alcohol, and Poor Diet
America runs on coffee — and that’s not entirely a good thing for sleep. Caffeine has a half-life of roughly five to seven hours, meaning that afternoon cup of cold brew you grabbed at 4 PM still has significant stimulant effects at 10 PM. Meanwhile, alcohol — often used as a sleep aid — actually fragments sleep architecture, reducing the quality of deep REM sleep. Add highly processed, sugar-heavy diets into the mix, and you have a lifestyle that is nutritionally incompatible with restful sleep.
Eszopiclone: What It Is and How It Helps
For people dealing with moderate to severe insomnia, physicians sometimes prescribe eszopiclone as part of a short-term treatment plan. Eszopiclone belongs to a class of medications known as sedative-hypnotics, which work by slowing activity in the brain to allow sleep to occur naturally.
Eszopiclone 2 mg tablet uses are primarily centered around helping adults who chronically can’t sleep fall asleep faster and stay asleep longer throughout the night. It’s typically prescribed for short-term use — usually one to two weeks — while the patient simultaneously works on behavioral and lifestyle changes that address the underlying causes of their insomnia.
Important Considerations:
- Eszopiclone is a prescription medication and should only be taken under the guidance of a licensed physician
- It is not a permanent solution — it addresses symptoms while other long-term strategies are implemented
- Side effects can include next-day drowsiness, so activities like driving should be approached with caution
- It should not be combined with alcohol or other central nervous system depressants
- Patients with certain medical conditions or on specific medications should consult their doctor before use
It’s worth noting that Eszopiclone 2 mg tablet uses are distinct from over-the-counter sleep aids, which typically rely on antihistamines and carry a different risk profile. Always consult a healthcare provider before starting any sleep medication.
Natural and Behavioral Strategies to Fight Insomnia
While medications like eszopiclone tablets can help in the short term, the most lasting solution to chronic insomnia is addressing the lifestyle factors driving it. Here are evidence-based strategies that sleep specialists across the United States recommend:
Cognitive Behavioral Therapy for Insomnia (CBT-I)
CBT-I is considered the gold-standard treatment for chronic insomnia by the American College of Physicians. It involves working with a therapist to identify and change the thoughts and behaviors that are keeping you awake. Studies show it is more effective long-term than medication alone.
Establish a Consistent Sleep Schedule
Going to bed and waking up at the same time every day — including weekends — is one of the most powerful things you can do to reset your circadian rhythm. Within a few weeks, your body will naturally begin to feel sleepy at the right time.
Create a Sleep-Friendly Environment
Your bedroom should be cool (around 65-68°F), dark, and quiet. Invest in blackout curtains, a white noise machine if you live in a noisy city like Chicago or New York, and a good quality mattress. Your brain should associate your bedroom exclusively with sleep and relaxation.
Limit Screen Exposure Before Bed
Power down all screens at least 60 to 90 minutes before bedtime. Use that time for relaxing activities — reading a physical book, light stretching, meditation, or journaling. This allows your melatonin levels to rise naturally and prepares your brain for sleep.
Manage Stress Proactively
Practices like mindfulness meditation, yoga, and deep breathing exercises have been clinically shown to reduce nighttime cortisol levels and ease the transition into sleep. Even 10 minutes of meditation before bed can significantly reduce the time it takes to fall asleep.
New Research: What Science Is Saying About Insomnia in 2024-2025
Recent studies coming out of Stanford University and Johns Hopkins have begun examining the link between social media algorithm exposure and increased insomnia rates in adults under 40. The research found that doom-scrolling — the habit of compulsively reading negative news feeds — activates the amygdala, the brain’s fear center, in ways that make it hard to fall asleep or stay asleep for hours afterward.
Additionally, new data from the American Sleep Association reveals that Americans living in areas with high light pollution — such as the greater Los Angeles basin and the New York metro area — report higher rates of insomnia compared to rural populations. The constant ambient glow of city lights is subtly but consistently disrupting melatonin production even through closed windows.
Researchers are also exploring the relationship between ultra-processed food consumption and sleep disruption. A 2024 study published in the journal Sleep Health found that individuals who consumed more than 50% of their daily calories from ultra-processed foods had significantly worse sleep quality and more frequent nighttime awakenings.
Frequently Asked Questions (FAQs)
Q1: What are the most common Insomnia symptoms I should watch for?
The most commonly reported Insomnia symptoms include difficulty falling asleep, waking up multiple times at night, feeling unrested after sleep even after a full night in bed, early morning awakening, daytime fatigue, mood disturbances, and difficulty focusing on tasks. If these symptoms occur three or more nights per week and persist for more than three months, you may be dealing with chronic insomnia.
Q2: How is eszopiclone different from over-the-counter sleep aids?
Eszopiclone is a prescription sedative-hypnotic that works directly on GABA receptors in the brain to induce sleep, while OTC options typically contain diphenhydramine (an antihistamine). Eszopiclone 2 mg tablet uses are specifically targeted at adults with clinical insomnia and are generally more effective for sleep maintenance. However, it requires medical supervision and carries specific warnings.
Q3: Can changing my lifestyle really cure my sleeplessness problem?
Absolutely — and research strongly supports this. For many people, the sleeplessness problem is a direct result of identifiable behavioral habits: irregular sleep schedules, excessive screen time, high caffeine intake, and unmanaged stress. Addressing these factors through CBT-I and lifestyle adjustments has been shown to produce long-term improvement in sleep quality without medication.
Q4: When should I see a doctor about not being able to sleep?
You should consult a physician when you experience disruptions in how you feel or function on a daily basis — meaning your insomnia is affecting your job performance, relationships, mood, or physical health. If you can’t sleep for more than three nights a week consistently over several weeks, it’s time to seek professional help. A sleep specialist can conduct proper assessments and discuss whether treatments like eszopiclone or CBT-I are appropriate for you.
Q5: Is insomnia more common in certain age groups in the US?
While insomnia can affect anyone, data from the National Sleep Foundation shows it is most prevalent in adults aged 30 to 60, particularly those in high-stress occupations and urban environments. However, it is increasingly diagnosed in younger adults and teenagers, largely driven by social media habits, academic pressure, and the always-on digital culture that defines life in cities like New York, Los Angeles, and Chicago.