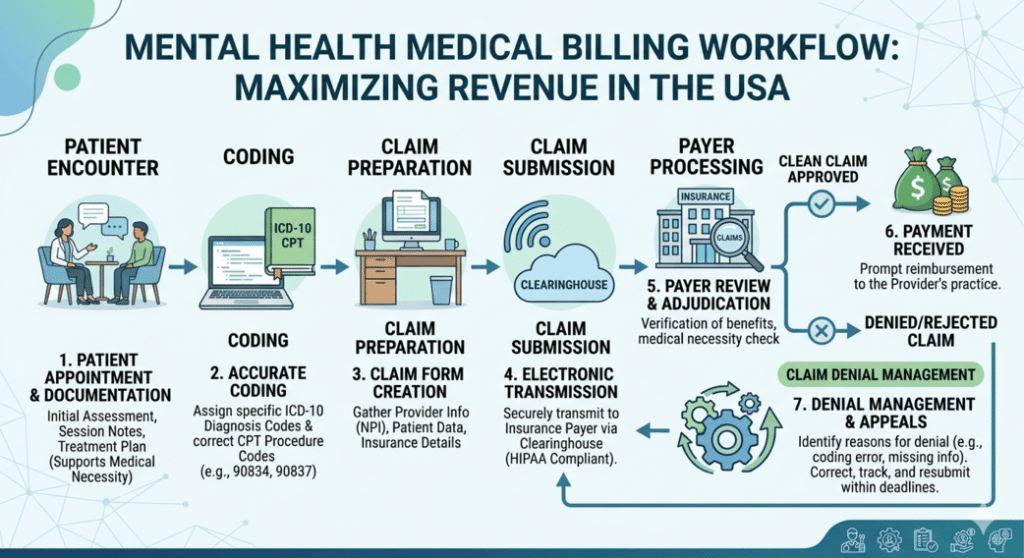
Running a mental health practice in Texas isn’t just about delivering quality care—it’s about navigating a billing system that can quietly drain your revenue if mishandled. Between evolving payer rules, prior authorization requirements, and the nuances of behavioral health coding, even experienced providers find themselves dealing with delayed payments or unexpected denials.
This is where mental health billing services Texas practices rely on become more than just administrative support—they become a strategic advantage. When billing is handled correctly, providers gain time, predictability, and financial clarity. When it isn’t, even a fully booked schedule can fail to translate into stable revenue.
Let’s break down what makes mental health billing uniquely complex, and how the right approach—or the right partner—can transform your practice.
Why Mental Health Billing Is Different From General Medical Billing
At first glance, billing might seem similar across specialties. But behavioral health operates under a distinct set of rules.
Mental health services often involve:
- Time-based CPT codes rather than procedure-based billing
- Frequent telehealth sessions with changing reimbursement policies
- Strict documentation requirements tied to medical necessity
- Variability in payer coverage for therapy vs psychiatry
For example, a therapist in Austin may provide a 60-minute psychotherapy session, but if documentation doesn’t align with payer expectations, reimbursement could be reduced or denied entirely. This is where mental health insurance billing services play a crucial role—ensuring every claim reflects both clinical accuracy and payer compliance.
The Real Cost of Billing Errors in Mental Health Practices
Small mistakes don’t stay small in revenue cycle management.
Consider this scenario:
A group practice submits claims without verifying insurance benefits in advance. Several sessions later, they discover the patient’s plan only covered a limited number of visits. The result? Retroactive denials and uncomfortable patient billing conversations.
This is a common issue—and one that a skilled mental health billing specialist would prevent through upfront eligibility checks.
Other costly issues include:
- Incorrect modifier usage for telehealth
- Missed timely filing deadlines
- Under-coding due to lack of documentation confidence
- Over-coding risks leading to audits
Each of these problems chips away at profitability. That’s why many practices now outsource mental health billing services instead of managing it in-house.
What High-Performing Practices Do Differently
Successful mental health providers don’t treat billing as an afterthought. They build systems around it.
They Prioritize Clean Claims
Clean claims—submitted correctly the first time—are the backbone of consistent cash flow. A mental health billing and coding company ensures that coding aligns with payer-specific rules, reducing rework and delays.
They Track Denials Like Data, Not Failures
Instead of reacting to denials, top practices analyze patterns. For instance, repeated denials for a specific CPT code might indicate a documentation gap or payer-specific rule change.
A strong mental health billing consultant helps identify these trends and fix them at the root.
They Invest in Specialized Expertise
General billing teams often lack behavioral health-specific knowledge. That’s why many providers work with a mental health billing services agency that understands therapy workflows, psychiatric billing, and compliance requirements in depth.
Should You Outsource Mental Health Billing?
It’s a question many Texas providers ask—and the answer depends on scale, complexity, and growth goals.
In-House Billing: When It Works
- Small solo practices with low claim volume
- Providers comfortable with coding and payer rules
- Minimal insurance-based revenue
Outsourced Billing: When It Makes Sense
As soon as your practice grows, billing complexity grows with it.
Outsourcing becomes valuable when:
- Denials are increasing
- Staff is overwhelmed
- Revenue cycles are inconsistent
- Expansion is planned
A reliable outsourced mental health billing partner doesn’t just submit claims—they manage the full lifecycle, from verification to payment posting.
What to Expect From a Professional Billing Partner
Not all billing providers offer the same level of service. The best mental health billing agency goes beyond basic claim submission.
Here’s what high-quality support looks like:
End-to-End Revenue Cycle Support
From patient eligibility checks to final reimbursement, a mental health billing provider should cover every step.
Expertise in Behavioral Health Coding
Accurate coding is critical. A seasoned mental health medical billing solution ensures proper use of CPT codes, modifiers, and diagnosis mapping.
Transparent Reporting
You should always know:
- What’s been billed
- What’s pending
- What’s denied—and why
Top mental health billing companies provide detailed, easy-to-understand reports.
Compliance and Risk Management
Regulations change frequently. A professional mental health billing agency stays updated to protect your practice from audits and penalties.
Real-World Example: Scaling Without Billing Chaos
A mid-sized therapy group in Dallas expanded from 3 to 12 providers within a year. Initially, they handled billing internally. As patient volume grew, so did their challenges:
- Claims backlog increased
- Denial rates crossed 20%
- Staff burnout became a concern
They transitioned to a top outsource mental health billing company, which implemented structured workflows and automated tracking.
Within six months:
- Denials dropped significantly
- Average reimbursement time improved
- Administrative workload reduced drastically
The key takeaway? Growth without billing support often leads to operational stress.
Choosing the Right Mental Health Billing Partner in Texas
Not every provider offering mental health medical billing services outsourcing will fit your practice.
Here’s how to evaluate your options:
Look for Behavioral Health Specialization
Avoid generalists. A professional mental health billing company understands therapy-specific challenges.
Ask About Technology Integration
Your billing partner should integrate with your EHR system for seamless data flow.
Evaluate Communication Style
Billing isn’t just backend work. You need a partner who communicates clearly and proactively.
Review Performance Metrics
Ask about:
- Average claim acceptance rate
- Denial resolution turnaround time
- Collection percentages
A reliable mental health billing and coding company will have measurable results to share.
The Growing Demand for Outsourced Mental Health Billing
Texas is seeing a rapid increase in demand for mental health services. With that growth comes administrative complexity.
More providers are turning to billing services for mental health providers that can handle:
- Multi-payer environments
- Telehealth billing regulations
- Insurance verification at scale
This shift isn’t just about convenience—it’s about sustainability.
Practices that rely on outsource mental health billing services often experience:
- Better financial forecasting
- Improved patient satisfaction
- Reduced operational risk
Common Pitfalls to Avoid
Even experienced providers make avoidable mistakes.
Ignoring Credentialing Delays
Without proper enrollment, claims won’t get paid. A strong system for credentialing is essential.
Overlooking Documentation Quality
Billing accuracy starts with clinical notes. Poor documentation leads to denials—even with correct coding.
Choosing Cost Over Expertise
Low-cost billing providers often lack specialization. This results in higher denial rates and lost revenue.
Where Billing Meets Practice Growth
Billing isn’t just about getting paid—it shapes how your practice grows.
When handled effectively, it allows providers to:
- Expand services confidently
- Hire new clinicians without revenue uncertainty
- Focus on patient care instead of paperwork
This is why many practices now see billing services for mental health therapists as an investment, not an expense.
FAQs
What makes mental health billing more complex than other specialties?
Mental health billing involves time-based coding, strict documentation requirements, and varying payer policies, making it more nuanced than standard medical billing.
When should I outsource mental health billing?
If your practice is growing, experiencing frequent denials, or struggling with revenue consistency, outsourcing becomes a practical solution.
How do mental health billing companies improve revenue?
They reduce claim errors, manage denials efficiently, and ensure compliance with payer rules, leading to faster and more reliable reimbursements.
Can a billing consultant help a small practice?
Yes. A mental health billing consultant can identify inefficiencies and optimize processes, even for smaller practices.
What should I look for in a billing provider?
Look for specialization in behavioral health, transparent reporting, strong communication, and proven performance metrics.
Final Thoughts: Building a Financially Strong Mental Health Practice
Mental health providers in Texas are doing critical work—but without the right billing systems, that work doesn’t always translate into financial stability. The increasing complexity of insurance policies and compliance requirements makes it essential to approach billing strategically.
Whether you manage it internally or partner with experts, the goal is the same: clean claims, faster reimbursements, and minimal revenue leakage.
This is where integrated support becomes valuable. Solutions that combine medical billing services, medical coding services, and complete medical billing and coding services help streamline operations. When paired with strong revenue cycle management and efficient credentialing services, practices gain a solid foundation for sustainable growth.
Organizations like 247 Medical Billing Services bring these elements together in a way that supports providers without disrupting their workflow. Rather than acting as just another vendor, they function as an extension of your practice—helping you stay focused on what matters most: delivering quality mental health care.
In a field where both clinical outcomes and operational efficiency matter, getting billing right isn’t optional—it’s essential.