Chronic skin conditions affect millions of people and often influence daily comfort, confidence, and quality of life. Many individuals feel confused when a skin problem continues for months or years despite careful skincare. As a medical professional working with dermatological conditions and preventive care, I frequently explain that the immune system plays a major role in many long-lasting skin disorders.
The immune system protects the body from infections, toxins, and harmful microorganisms. However, immune responses can sometimes become overactive or misdirected. When this occurs, the skin may develop persistent inflammation, rashes, or lesions that return repeatedly. The immune system affects the skin can help patients recognise triggers, manage symptoms, and seek appropriate care. This article explains how immune activity contributes to chronic skin disorders and how lifestyle, nutrition, and medical care can support healthier skin.
The Skin and the Immune System Work Closely Together
The skin acts as the body’s first line of defence. It blocks harmful bacteria, viruses, and environmental irritants from entering the body. Beneath the surface, immune cells monitor the skin for potential threats.
Several types of immune cells live within the skin, including:
- T-cells
- Dendritic cells
- Macrophages
- Mast cells
These cells identify harmful organisms and trigger protective responses. When the immune system detects danger, it releases chemicals that create inflammation. This process helps remove harmful substances and begin healing.
Inflammation often produces redness, warmth, swelling, and itching. In a healthy situation, this response fades once the threat disappears. However, chronic skin disorders occur when the immune response continues even after the original trigger has gone.
What Causes Immune Imbalance in the Skin
The immune system normally maintains a careful balance. It reacts strongly to infections while avoiding damage to healthy tissues. In chronic skin disorders, that balance becomes disrupted.
Several factors may contribute to immune imbalance:
- Genetic predisposition
- Environmental exposure
- Hormonal changes
- Stress
- Microbial imbalance
- Nutritional deficiencies
Because many of these factors interact with each other, the exact cause of a chronic skin condition can remain unclear. The immune system may continue producing inflammation even when no obvious external trigger exists.
Chronic Skin Disorders Linked to Immune Activity
Many well-known skin conditions develop partly because of immune system activity. These conditions involve inflammation that persists over time.
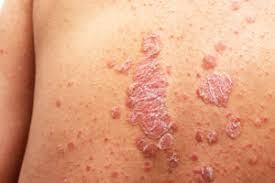
Psoriasis
Psoriasis develops when immune cells stimulate skin cells to grow much faster than normal. This rapid growth creates thick, scaly plaques that may itch or feel sore. The condition often appears on elbows, knees, scalp, and lower back.
Psoriasis flare-ups may occur after infections, stress, or skin injuries. However, flare-ups can also occur without any clear trigger.
Eczema (Atopic Dermatitis)
Eczema involves immune reactions that weaken the skin barrier and increase sensitivity. People with eczema often experience dry, itchy skin that becomes inflamed after contact with irritants or allergens.
The immune system in eczema reacts strongly to substances that usually cause no harm. This exaggerated response leads to chronic itching and inflammation.
Granuloma Annulare
Granuloma annulare produces ring-shaped patches or raised lesions on the skin. Doctors believe immune responses within the skin trigger these lesions, although the exact cause remains uncertain.
Some patients explore supportive approaches that combine medical advice with lifestyle strategies. For example, people interested in complementary options often read about Herbal Supplements for Granuloma Annulare as part of wider discussions on skin health and immune balance.
Lupus-Related Skin Conditions
Lupus is an autoimmune disease in which the immune system attacks healthy tissues. Many individuals with lupus develop skin symptoms, including facial rashes and sensitivity to sunlight.
Autoimmune diseases highlight how powerful immune responses can affect multiple parts of the body, including the skin.
Why Chronic Skin Disorders Flare Up
People with chronic skin conditions often notice periods when symptoms worsen. These episodes, called flare-ups, usually occur when the immune system becomes more active.
Common triggers include:
- Emotional stress
- Illness or infection
- Skin injury
- Changes in weather
- Certain medications
- Poor sleep
During a flare-up, immune cells release inflammatory chemicals such as cytokines. These chemicals increase blood flow and stimulate skin cells, producing redness, swelling, and itching.
Identifying personal triggers can help reduce flare-ups and maintain more stable skin health.
The Role of Inflammation
Inflammation forms a central feature of many chronic skin disorders. Although inflammation protects the body during infections, excessive or prolonged inflammation damages healthy tissue.
In chronic skin disease, inflammatory signals continue circulating in the skin. This ongoing activity may produce:
- Thickened skin patches
- Persistent redness
- Scaling or flaking
- Itching and discomfort
Long-term inflammation may also weaken the skin barrier, allowing irritants and microbes to enter more easily. This cycle can maintain the condition unless treatment interrupts the inflammatory process.
The Skin Microbiome and Immune Balance
The skin contains a natural community of microorganisms known as the microbiome. These microorganisms include beneficial bacteria that support the skin’s protective functions.
The immune system interacts closely with the microbiome. Healthy bacteria help regulate immune responses and prevent harmful microbes from multiplying.
However, certain factors can disturb this microbial balance:
- Harsh soaps or cleansers
- Excessive antibacterial products
- Antibiotic use
- Environmental pollution
- Skin injuries
When microbial balance shifts, the immune system may react more aggressively. This reaction can worsen chronic skin inflammation.
How Stress Influences the Immune System
Emotional stress can strongly affect immune activity. Stress hormones such as cortisol alter immune cell behaviour and increase inflammation within the body.
Many patients notice that stressful periods lead to skin flare-ups. This connection occurs because stress can:
- Increase inflammatory chemicals
- Reduce skin barrier strength
- Delay skin healing
- Alter microbial balance
Managing stress through relaxation techniques, physical activity, and adequate sleep often improves overall skin stability.
Nutrition and Immune Health
Nutrition plays an important role in immune function. The immune system depends on vitamins, minerals, and healthy fats to regulate inflammation and maintain balanced responses.
Several nutrients support skin and immune health:
- Vitamin A for skin repair
- Vitamin C for collagen production
- Vitamin D for immune regulation
- Zinc for wound healing
- Omega-3 fatty acids for inflammation control
Poor diet or nutrient deficiencies may worsen inflammatory skin conditions. Improving dietary habits often helps support long-term skin health.
Some individuals choose to include supplements alongside dietary improvements. For example, people researching supportive lifestyle approaches may read about Granuloma Annulare Natural Treatment options that include nutrition, stress management, and targeted supplementation.
Before beginning supplements, discussing options with a healthcare professional helps ensure safe and appropriate use.
The Importance of the Skin Barrier
The outermost layer of skin forms a protective barrier that prevents moisture loss and blocks irritants. Chronic skin disorders often weaken this barrier.
A weakened skin barrier may lead to:
- Dryness
- Increased sensitivity
- Greater risk of infection
- Persistent irritation
Supporting the skin barrier remains a key part of managing chronic skin disease. Gentle skincare products, regular moisturising, and avoiding harsh chemicals can help restore barrier strength.
Medical Treatments That Target the Immune System
Modern dermatology offers several treatments that reduce immune-driven inflammation in chronic skin disorders. Doctors select treatment based on the severity of symptoms and the specific condition involved.
Common medical approaches include:
Topical corticosteroids
These creams reduce inflammation and itching.
Calcineurin inhibitors
These medications suppress immune activity in the skin.
Phototherapy
Controlled exposure to ultraviolet light helps regulate immune responses.
Biologic medications
These advanced therapies target specific immune pathways involved in conditions such as psoriasis.
Medical treatment aims to reduce inflammation, improve comfort, and prevent long-term skin damage.
Lifestyle Habits That Support Immune Balance
Although medication may be necessary for many chronic skin conditions, daily habits can also support immune balance and skin health.
Helpful lifestyle practices include:
Consistent skincare routines
Use gentle cleansers and moisturisers that protect the skin barrier.
Balanced nutrition
Include fresh vegetables, fruit, whole grains, and healthy fats.
Adequate sleep
Sleep supports immune regulation and skin repair.
Stress management
Regular physical activity, meditation, or relaxation exercises can reduce inflammatory responses.
Sun protection
Excess sun exposure can worsen certain immune-related skin conditions.
Some people also seek nutritional supplements to support overall health. Reliable sources that provide Best Vitamins and Supplements Products Online UK help individuals choose quality products that meet recognised safety standards.
When to Seek Medical Advice
Chronic skin conditions can sometimes resemble other health problems. Professional evaluation ensures an accurate diagnosis and appropriate treatment.
Medical advice is important if you notice:
- Skin symptoms that last several weeks
- Rapidly spreading rashes
- Painful or swollen lesions
- Signs of infection such as pus or fever
- Skin symptoms affecting daily activities
Early medical care can prevent complications and help identify suitable treatment options.
Living With Chronic Skin Disorders
Chronic skin conditions often involve cycles of improvement and flare-ups. Many patients feel frustrated during periods when symptoms return unexpectedly.
A practical approach includes:
- Following treatment plans consistently
- Maintaining gentle skincare routines
- Tracking potential triggers
- Supporting immune health through diet and lifestyle
- Seeking medical advice when symptoms change
With appropriate care and lifestyle adjustments, many people manage chronic skin disorders successfully and maintain good quality of life.
Final Thoughts
The immune system plays a central role in many chronic skin disorders. Immune cells within the skin protect the body from infection, yet these cells can sometimes trigger persistent inflammation.
Conditions such as psoriasis, eczema, and granuloma annulare often involve immune responses that continue beyond their protective purpose. Genetics, stress, environmental exposure, microbial balance, and nutrition all influence how the immune system behaves.
Although the exact cause of some chronic skin conditions remains uncertain, a combination of medical treatment, healthy habits, and supportive lifestyle strategies often leads to improvement. If symptoms persist or worsen, professional guidance can help identify effective treatment and provide reassurance.